For many people, “backache” is just part of daily life: a dull pull when you wake up, a burn after long sitting, or a tight knot when you bend. But behind that familiar ache, the real story often lies in your low back pain muscles—not only in discs, nerves, or bones.
These deep and superficial muscles carry your body weight, control every bend and twist, and react instantly to stress. When they’re overloaded, weak, stiff, or poorly coordinated, you don’t just feel discomfort; your brain quietly starts to protect the area. Movements feel risky, simple tasks become exhausting, and you may begin to avoid things you used to enjoy.
The tricky part? Most scans only show bones, joints, and discs. They rarely capture how your low back pain muscles are actually working. That’s why many people come away from imaging with “nothing serious found” but still struggle to sit, stand, or sleep without pain.
In this in-depth guide, we’ll explore:
- Which muscles support your lower back
- Hidden reasons they become painful and overprotective
- How to tell muscle pain from nerve pain
- Practical, stepwise strategies to reset, strengthen, and protect them
- When self-care is enough—and when to seek professional help
By the end, you’ll understand your low back not as something “fragile,” but as a system you can train, calm, and build up again.
Why low back pain muscles matter more than you think
When people hear “slipped disc” or “pinched nerve,” they immediately get worried. When they hear “muscle strain,” it sounds less serious. In reality, low back pain muscles are often the main reason your back keeps hurting, even when scans look relatively normal.
Muscles are your spine’s first line of defense
The muscles around your lower spine:
- Keep you upright against gravity
- Share load with discs and joints
- React to tiny changes in balance
- Protect sensitive structures when something feels “off”
When they work well, you can bend, lift, twist, and sit with confidence. When they don’t, the body starts using backup strategies—gripping, bracing, and avoiding movement—that make pain worse over time.
Pain without visible damage
Many people with chronic back issues have:
- Normal or age-expected disc and joint changes on imaging
- No single “big” structural problem
- Significant pain, stiffness, and fear of movement
In these cases, the issue is less “a broken spine” and more a sensitized system: muscles guarding too hard, nerves on high alert, and the brain expecting danger whenever the low back moves. Calming and retraining those muscle patterns often gives more relief than focusing only on scans.
Meet the key muscles in your lower back
When we talk about low back pain muscles, we actually mean a whole team that wraps around your lumbar spine, pelvis, and hips. They work together like cables, guy ropes, and springs.
Main muscle groups involved
| Muscle group | Where you feel it | Main job | How it can misbehave |
|---|---|---|---|
| Erector spinae | Long muscles running alongside the spine | Keep you upright, extend the back | Get tired and overworked with long sitting/standing |
| Multifidus | Short, deep muscles between vertebrae | Fine-tune segmental stability | Switch off after injury or pain, leading to wobbliness |
| Quadratus lumborum (QL) | Deep on each side, between lower ribs and pelvis | Side-bending, pelvic stability when walking | Becomes tight and tender, often causing one-sided ache |
| Gluteus maximus/medius | Buttock muscles | Hip extension and side stability | Weakness shifts load into the small lumbar muscles |
| Hip flexors (psoas, iliacus) | Front of hip and deep inside the pelvis | Lift the leg, contribute to posture | Tightness pulls the spine into more arch and compression |
| Abdominals & deep core | Front and sides of the trunk | Support and brace the trunk, assist breathing | Poor timing or weakness forces the back to work overtime |
When any part of this network is weak, tight, or late to activate, the remaining low back pain muscles try to “help” by gripping and working harder than they should. That’s when you feel knots, spasms, and deep fatigue.
How lower back muscles talk to your brain
Muscles are not just pieces of meat that shorten and lengthen; they are full of sensors sending nonstop messages to your nervous system.
Sensory traffic from your low back
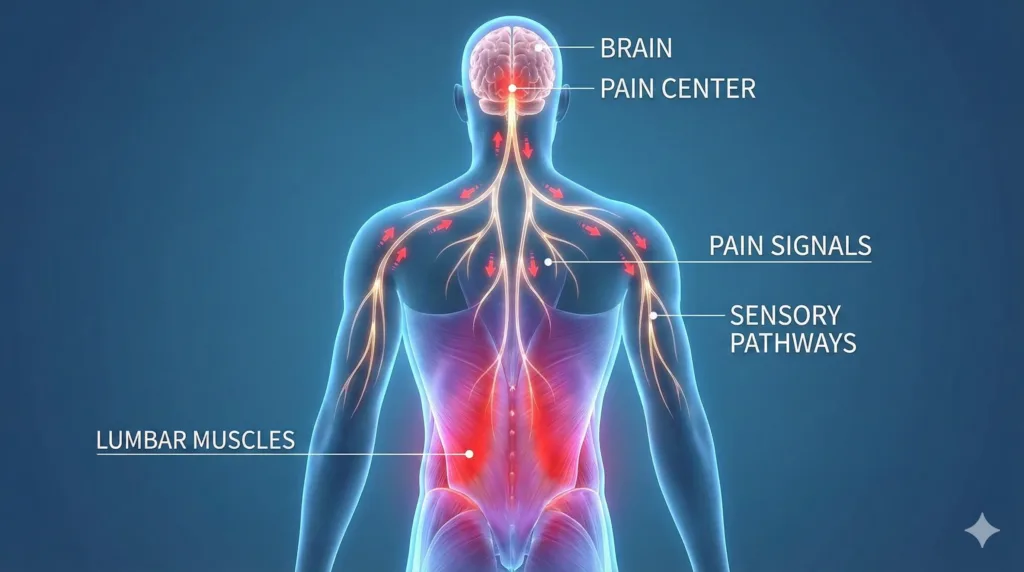
Inside the muscles around your spine are receptors that:
- Sense stretch and length
- Detect tension and load
- Report speed and direction of movement
These signals help your brain decide:
- Is this movement safe?
- Do we need to protect something?
- How much force should we generate?
If your low back pain muscles have been strained, overloaded, or painful for a while, the brain may start to interpret normal signals as threatening. This leads to:
- Extra muscle guarding and stiffness
- Pain with lighter loads than before
- A “fragile back” feeling even when tissues are healing
The result is a loop: pain → guarding → less movement → more sensitivity → more pain. Breaking that loop is one of the main goals of good rehab.
Hidden causes inside your low back muscle system
Some causes are obvious—a single heavy lift, a fall, an awkward twist. Others are slow, sneaky, and cumulative.
1. Micro-overload and repetitive strain
You don’t need to move furniture or deadlift huge weights to overload the lower back. Everyday micro-stresses add up:
- Repeated bending and twisting at work
- Lifting children or bags without using the hips
- Doing housework in a bent posture for long periods
- “Weekend warrior” sports after sitting all week
Each time, the muscles around your lumbar spine get a little more irritated. If rest and recovery are too short, they never fully settle. Over weeks and months, the area becomes tender and reactive.
2. Guarding and muscle spasm
When your brain feels that the spine might be at risk—because of a sudden twinge, an old injury, or fear of movement—it often tightens the muscles around the area like a splint.
Short-term guarding can help you avoid a bigger injury. But if your low back pain muscles stay in protective mode for too long, you may notice:
- Hard, rope-like bands alongside the spine
- Sharp grabs of pain with simple motions
- Reduced flexibility and a feeling of “stuckness”
Over time, this constant guarding reduces blood flow and oxygen supply, making the muscles even more irritable.
3. Trigger points and referred pain
Trigger points are small, hyper-sensitive spots within a tight muscle band. Pressing on them can reproduce your familiar pain and sometimes send it somewhere else.
Common patterns:
- Trigger points in the QL can cause aching in the flank or top of the pelvis
- Trigger points in gluteal muscles can mimic sciatic-type pain down the leg
- Trigger points in lumbar extensors can cause a band of pain across the belt line
Because referred pain can travel, people often think these sensations mean a disc is “slipped” when in fact the main driver is muscle.
4. Muscle imbalance patterns
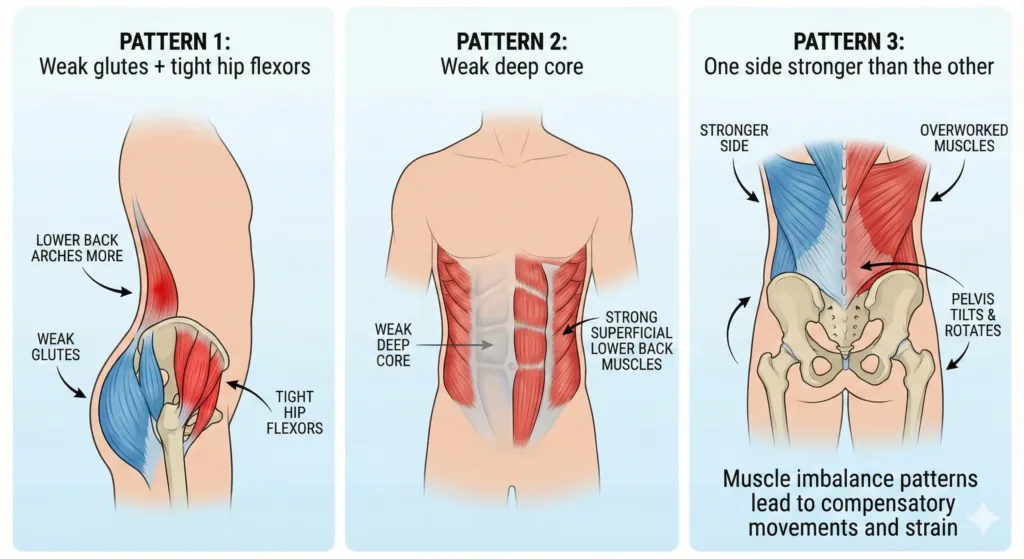
Your body chooses movement patterns based on habit and strength, not just perfect anatomy. Common imbalances that overload the lower back include:
- Weak glutes + tight hip flexors → the lower back arches more, and spinal muscles must control every step
- Weak deep core → superficial back muscles grip harder just to keep you upright
- One side stronger than the other → the pelvis tilts and rotates, forcing certain muscles to work overtime
These are hidden causes: they rarely show on scans, but they truly shape how your low back pain muscles feel during daily life.
Everyday habits that quietly overload low back pain muscles
Most people do not injure their back in the gym. They provoke their low back pain muscles with the way they sit, stand, sleep, and manage stress.
Sitting: “the slow leak” of spinal energy
Long sitting periods can:
- Shorten hip flexors, tilting the pelvis
- Stretch and tire the spinal muscles in a rounded posture
- Reduce circulation in the tissues of the lumbar area
Signs your sitting habits are a problem:
- Aching after 20–30 minutes at a desk
- Feeling better when you get up and walk for a minute
- Stiffness or burning in the belt area when you stand after sitting
Small changes—like regular posture breaks, a slight lumbar support, and placing feet flat on the ground—can ease the load dramatically.
Standing still for too long
Standing can be just as stressful when it’s static:
- You lock your knees and arch the back
- You lean on one leg more than the other
- You clench your buttocks and back for support
Over time, this constant mild contraction keeps the low back pain muscles in a semi-guarded state. Gentle weight shifting, micro-movements, and occasional walking breaks help more than you might think.
Sleep position and mattress
Night is when your body repairs. If your position keeps the spine twisted or sagging, the lower back never gets a true break.
Typical issues:
- Stomach sleeping with the neck and low back rotated
- Side sleeping without a pillow between the knees, twisting the pelvis
- A mattress that is too soft or worn out, letting the hips sink and the lumbar area collapse
Neutral alignment—where your ears, shoulders, and hips are roughly in one line—is friendlier to the muscles supporting your lower back.
Stress, emotions, and muscle tone
Stress doesn’t “just” affect mood; it also raises background muscle tension. You might:
- Clench your jaw
- Tighten your shoulders
- Grip around the lower back without realizing
If this is constant, low back pain muscles become hypersensitive and tire quickly. Learning to regulate stress—through breathing, relaxation, and enjoyable movement—often reduces pain even when nothing else has changed.
Muscle pain or nerve pain: how to tell the difference
Distinguishing between muscle-dominant pain and nerve-driven pain is important. You can have both at the same time, but the patterns differ.
Features suggesting muscle-dominant pain
Pain likely comes mainly from muscles when:
- Discomfort is mostly in the low back, sometimes into the buttocks or upper hips
- Pressing on the area reproduces the familiar ache
- Pain feels like tightness, cramping, pulling, or a deep dull ache
- Symptoms often improve with gentle movement and worsen with long sitting or standing in one position
In these cases, carefully working on low back pain muscles—mobility, strength, and endurance—usually helps significantly.
Features suggesting nerve involvement
You may have more than a muscle problem if you notice:
- Sharp, electric, shooting, or burning pain running down a leg
- Numbness, tingling, or pins-and-needles in a clear line
- Weakness in the foot or leg (tripping, difficulty lifting the toes or heel)
- Changes in bladder or bowel control
- Sudden severe pain after a fall, accident, or heavy trauma
These signs call for prompt medical assessment. Muscles will still need rehab, but the underlying nerve or structural issue must be checked first.
Simple home self-checks for your lower back muscles
These quick checks do not replace a professional exam, but they can give you clues about how your low back pain muscles behave.
1. Forward bending comfort

- Stand with feet hip-width apart.
- Slowly fold forward, letting your arms hang.
Notice:
- Does one side of the lower back feel tighter or more protective?
- Is the pull more in muscles or in the center of the spine?
- Does a slight bend of the knees make it easier?
2. Gentle backward lean

- Place your hands on your hips or small of the back.
- Gently lean backward, only within comfort.
Ask yourself:
- Do you feel compression or pinching in one specific spot?
- Is the sensation more like tight muscles stretching?
- Does supporting yourself with your hands reduce the discomfort?
3. Side-bending symmetry

- Slide one hand down the outside of the thigh while bending sideways.
- Repeat on the other side.
Compare:
- Is one side stiff, blocked, or painful?
- Does the pain sit over the QL area (between ribs and pelvis)?
4. Basic endurance hold

- Lie on your stomach with a folded towel under your forehead.
- Gently squeeze the buttocks and lightly brace your core.
- Lift the upper chest a few centimeters off the surface, without straining the neck.
Hold for up to 10–15 seconds, if comfortable.
If your low back pain muscles shake or fatigue very quickly, or if they cramp immediately, it suggests low endurance and a tendency to over-protect. That’s exactly what a gradual strengthening plan can improve.
Stop any test that causes sharp shooting pain, strong leg symptoms, dizziness, or feeling unwell.
A stepwise reset plan for low back muscle pain
Think of this as a roadmap. It does not replace individualized care, but it reflects common principles used in good rehabilitation.
Stage 1: Calm and unload
Goal: reduce guarding so your low back pain muscles can start moving more freely.
Helpful positions
- Legs-up rest: Lie on your back with your lower legs supported on a chair or sofa, hips and knees at roughly 90°. This reduces pressure on discs and allows muscles to relax.
- Side-lying with pillow: Lie on your side with a pillow between the knees and ankles so the pelvis stays neutral.

Gentle movements
- Pelvic tilts: In lying, gently rock the pelvis forward and backward within comfort.
- Knee rolls: With knees bent, slowly let them drift side to side, only as far as feels safe.
- Diaphragmatic breathing: One hand on the chest, one on the belly. Inhale into the lower ribs and belly, exhale slowly, letting the back soften.
The aim here is “easy, smooth movement,” not stretching to the maximum.
👨⚕️ Dr. Arora’s Clinical Note:
Many patients ask me if they should “stretch the tight spot” when the back feels locked or guarded. Counter-intuitively, long end-range stretches can increase protective muscle spasm because your nervous system interprets it as a threat.
A more reliable way is isometric analgesia (pain-calming holds): pick the direction that feels even slightly easier (often a supported hip-hinge at a kitchen counter, or a very small backward lean), then do a light 20–30% effort hold for 8–10 seconds, rest 5 seconds, repeat 5–6 rounds.
If your bending/standing feels freer or your pain drops even one level, you’ve essentially “reset” guarding—then your cat–camel, knee rolls, and hip mobility work tends to land better. If symptoms spike or you feel sharp, shooting leg pain, skip the hold and return to Stage 1 unloading + short, frequent walks.
Stage 2: Restore mobility
Once pain is a little calmer, movement helps nourish joints and tissues.
Cat–camel (spinal mobility)
On hands and knees, alternate between gently rounding and arching the back. Move slowly, syncing with your breath, and stay away from sharp pain.
Single and double knee-to-chest
On your back, bring one knee towards the chest, hold 10–15 seconds, then switch. If comfortable, you can later try both knees together. Avoid if it strongly aggravates leg pain.
Hip flexor stretch
In a half-kneeling position (one knee on the floor, the other foot forward), gently shift the pelvis forward until you feel a stretch at the front of the hip, not in the lower back. This helps reduce the pull of tight hip flexors on the spine.
Stage 3: Strengthen and coordinate
Now the goal is to teach the trunk and low back pain muscles to share load with the core and hips.
Abdominal brace with breathing
- Lie on your back with knees bent.
- Inhale gently, expanding the belly and ribs.
- As you exhale, lightly tighten the lower tummy as if zipping up snug pants.
You should feel gentle firmness around the waist, not a hard breath-holding brace.
Glute bridge
- From the same position, press your heels into the floor.
- Lift your hips until your body forms a straight line from shoulders to knees.
- Focus on the buttocks doing most of the work while the lower back feels supported, not pinched.
Hold 3–5 seconds, lower slowly. Start with 8–10 reps.
Bird-dog
- On hands and knees, lightly brace the core.
- Reach one arm forward and the opposite leg backward.
- Keep hips level, avoiding twisting or sagging.
Hold 5–10 seconds, then switch sides. This trains stability and control, so the low back pain muscles work in coordination rather than in isolation.
Side-lying clamshell
- Lie on your side with hips and knees bent, feet together.
- Keep feet touching while lifting the top knee slightly.
This targets the gluteus medius, crucial for hip and pelvic stability, reducing strain on the lumbar area.
Aim for 2–3 sets of 8–15 repetitions per exercise, most days of the week, as tolerated.
Stage 4: Integrate into daily life
Exercise sessions alone are not enough if daily habits keep irritating the area. Now you apply these gains to real-world tasks.
Lifting in daily life
- Feet slightly apart, load kept close to the body
- Hinge at hips and knees rather than rounding from the waist
- Light core brace as you lift, then release as you set the object down
Desk strategy
- Change position at least every 25–30 minutes
- Alternate between sitting and standing if possible
- Take mini-walks or stretch breaks to give the lower back fresh blood flow
General activity
Regular moderate activity—like walking, swimming, or cycling—helps your low back pain muscles build endurance, improves mood, and keeps joints nourished.
When low back pain needs expert help
Most back pain episodes related mainly to muscle settle with time, lifestyle changes, and proper loading. But some situations need professional assessment.
Red-flag signs (seek urgent medical help)
Get prompt medical care if your back pain is accompanied by:
- Recent significant trauma (fall, accident, heavy blow)
- Fever, chills, or feeling very unwell
- Unexplained weight loss
- History of cancer, serious infection, or immune suppression
- New problems with bladder or bowel control
- Progressive leg weakness, numbness, or loss of coordination
These can indicate something more serious than isolated low back pain muscles and require timely evaluation.
When persistent symptoms need rehabilitation
Consider seeing a physiotherapist or similar professional if:
- Pain or stiffness lasts more than 4–6 weeks
- You experience frequent flare-ups from small triggers
- You feel fearful or confused about which movements are safe
- You’ve tried rest alone and it hasn’t helped
A good rehab program looks at posture, movement patterns, muscle strength, endurance, and your beliefs about pain. It doesn’t just treat one muscle—it retrains how your entire system works.
For deeper, evidence-based reading, start with NIAMS and NINDS patient resources, and for rehab decisions follow the 2021 physical therapy guideline: [Interventions for the Management of Acute and Chronic Low Back Pain: Revision 2021, 2021]
For deeper medical information on back pain, many professionals refer to educational resources from organizations like the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS) and the National Institute of Neurological Disorders and Stroke (NINDS), which explain how discs, joints, nerves, and muscles all interact.
Long-term prevention blueprint for low back pain muscles
Once your back starts to feel better, it’s tempting to “forget about it.” But maintenance is what keeps your low back pain muscles resilient.
Daily movement minimum
- Break up sitting with short bouts of walking or standing
- Include some form of light to moderate exercise most days
- Keep a small routine of spine-friendly mobility and strength moves (bridges, bird-dog, hip stretches) several times per week
Load management
- Increase training or workload gradually, especially after periods of inactivity
- Rotate tasks—avoid doing the same bending or lifting pattern for hours
- Listen to early warning signs: mild tightness or fatigue is a cue to pause and reset, not to panic
Recovery and sleep
- Aim for consistent, good-quality sleep so your tissues can repair
- Use supportive sleeping positions that keep your lower back neutral
- Avoid testing your limits with heavy lifting or new high-load activities when you’re very tired or run down
Mindset shift
Perhaps the most powerful prevention tool is how you think about your back. Instead of seeing it as fragile, see it as trainable:
- Pain does not always mean damage
- Movement, done gradually and wisely, is usually medicine for muscles
- Strong, coordinated low back pain muscles are your allies, not your enemies
With the right information and habits, your lower back can become something you trust again—supporting not just basic tasks, but the activities you love.
FAQs about low back pain muscles
1. What exactly are low back pain muscles?
Low back pain muscles are the group of muscles around your lumbar spine and pelvis that stabilize and move your lower back. They include the multifidus, erector spinae, quadratus lumborum, glutes, hip flexors and deep core. Together they control everyday movements, share load with discs and joints, and can become painful when they’re strained, weak, tight or poorly coordinated.
2. Can low back pain muscles cause pain even if my MRI is normal?
Yes, your muscles can cause significant low back pain even when your MRI looks normal. Imaging mainly shows bones, discs and major structural problems, not how irritated or overworked the muscles and soft tissues are. Strain, trigger points, fatigue and protective guarding can all create pain, stiffness and restricted movement even with “age-appropriate” or normal scans.
3. How can I tell if my pain is from low back pain muscles or from a nerve?
Pain coming mainly from low back pain muscles usually feels like aching, tightness, pulling or cramping in the lower back or buttocks and often eases with gentle movement. Nerve pain is more likely to be sharp, electric, burning or shooting down the leg, sometimes below the knee, and can come with numbness, tingling or weakness. If you notice strong leg symptoms, bladder or bowel changes, or progressive weakness, you should seek medical advice promptly.
4. Is exercise safe when my low back pain muscles are sore?
In most cases, gentle, well-chosen exercise is safe and actually helps low back pain muscles recover. The key is to start with low-load movements your back tolerates well—such as short walks, pelvic tilts or simple core activation—and build up gradually. Avoid pushing into sharp or worsening pain, and reduce intensity or modify exercises if symptoms spike; if you’re unsure what’s appropriate, a professional assessment is useful.
5. Which exercises are best to strengthen low back pain muscles?
The best exercises for low back pain muscles are those that work the whole trunk and hips rather than isolating one small area. Examples include abdominal bracing with breathing, glute bridges, bird-dog, side-lying clamshells and gentle back extensions. These moves encourage your lower back muscles to share load with the core and glutes, improving stability and reducing the chance that one overworked area keeps flaring.
6. How long do low back pain muscles take to recover after a strain?
Mild strains in low back pain muscles may settle within a few days to a couple of weeks, while more significant muscle injury can take several weeks to feel normal. Recovery speed depends on factors like general health, sleep, stress levels and how quickly you introduce the right mix of rest and graded movement. Continuing strength and endurance work even after the pain eases helps make these muscles more resilient and less likely to flare again.
7. Can poor posture really lead to low back pain muscles hurting?
Poor posture alone doesn’t “damage” your spine, but staying in one position too long can overload certain muscles and joints. Rounded sitting, prolonged static standing or twisted, asymmetrical positions gradually increase strain on low back pain muscles. Changing positions regularly, hinging from the hips instead of bending from the waist, and keeping loads close to the body are more important than trying to hold one perfect posture all day.
8. Do tight hamstrings affect low back pain muscles?
Yes, very tight hamstrings can indirectly stress low back pain muscles. When the hamstrings limit hip flexion, your spine has to move more to achieve the same bend, which can fatigue and irritate the tissues in the lower back. Gentle, regular hamstring stretching combined with hip and glute strengthening often improves movement patterns and reduces that extra load on the lumbar area.
9. Can stress and anxiety make low back pain muscles worse?
Stress and anxiety can definitely make low back pain muscles feel tighter and more painful. Elevated stress levels increase baseline muscle tension and make the nervous system more sensitive, so normal signals from your back can be interpreted as more threatening. Combining physical strategies like exercise, mobility and pacing with stress-management tools such as breathing exercises, relaxation techniques and enjoyable activities often leads to steadier, longer-lasting relief.
10. When should I worry that my low back pain muscles are a sign of something serious?
Most muscle-related low back pain is not dangerous and improves with time, movement and lifestyle changes. You should seek medical assessment, however, if your pain comes with red-flag signs such as recent major trauma, fever, unexplained weight loss, history of cancer or serious infection, changes in bladder or bowel control, or progressive weakness or numbness in the legs. These situations need a careful check-up to rule out conditions beyond low back pain muscles alone.




